Breaking the ADHD Stigma: Promoting Awareness and Understanding
Hello Therapyden, LPC on Jul 13, 2023

ADHD Statistics
Everyone might occasionally experience challenges with staying still, maintaining focus, or reining in impulsive actions. For some people, these challenges extend beyond occasional inconveniences. They are overwhelming that it disrupts daily life, affects academic performance, impacts relationships, and impedes personal growth. Individuals of this nature may be diagnosed with Attention-Deficit/Hyperactivity Disorder (ADHD), a neurodevelopmental condition typically identified during childhood that persists into adulthood.
ADHD manifests in a variety of ways, and symptoms can change over time. Typically, it is characterized by persistent patterns of inattention, hyperactivity, and impulsivity. These are not occasional slips but consistent behaviors that are more severe and frequent than what is usually observed in individuals at a comparable level of development.
Global Prevalence of ADHD

ADHD affects individuals across the world, irrespective of geographical location or cultural background. According to a study conducted in 2020, the global prevalence of adult ADHD is estimated to be around 2.8%. Recent findings also indicate that ADHD affects approximately 7.6% of children aged 3 to 12 years, while the prevalence among teenagers aged 12 to 18 is approximately 5.6%.
Comparison of ADHD Prevalence Among Different Countries
Every country around the world experiences the prevalence of ADHD differently. These variations can be attributed to a multitude of factors, including cultural differences, healthcare systems, diagnostic practices, and environmental influences.
France: In France, ADHD is referred to as "TDAH" (Trouble déficit de l'attention/hyperactivité) and impacts both children and adults. According to a study, the diagnosis of ADHD in children and adolescents experienced a significant increase of 96% between 2010 and 2019. It is observed that ADHD diagnoses are more prevalent in boys than in girls. Notably, in 2017, approximately 50.6% of children who were hospitalized with an ADHD diagnosis also had another psychiatric condition. The utilization of methylphenidate (MPH) treatment among hospitalized children diagnosed with ADHD varied between 56.4% and 60.1% during the study period.
Ireland: ADHD has a significant impact on the population of Ireland, with approximately 5% of individuals being affected by the disorder. Data from the Central Statistics Office in Ireland (CSO) indicates that ADHD is more prevalent in boys than in girls, with boys being diagnosed with ADHD approximately four times more frequently than girls. This gender disparity is further supported by the CSO's findings, which report that nearly twice as many boys between the ages of 5 and 19 experience difficulties related to learning, memory, or concentration compared to girls.
Mexico: ADHD exhibits a high prevalence rate, with an estimated 3-5% of school-age children qualifying for a diagnosis. In Mexico alone, this accounts for approximately 1.5 million cases, signifying a significant burden. Moreover, within clinical pediatric settings, ADHD constitutes over 30% of all reported cases. Alarmingly, reports from health services indicate a substantial time gap of around 8 to 15 years between the identification of symptoms and the initiation of treatment for individuals with ADHD.
The Netherlands: According to a study conducted by Cambridge University, the estimated prevalence rate of ADHD in the Netherlands (meeting the full diagnostic criteria) among older adults was found to be 2.8%. Additionally, the study reported a prevalence rate of 4.2% for symptomatic ADHD (exhibiting significant ADHD symptoms without meeting the full criteria). Notably, the research found that younger elderly adults, aged 60 to 70 years, reported a significantly higher number of ADHD symptoms compared to older elderly adults aged 71 to 94 years.
Belgium: In the Belgian population, the estimated prevalence of ADHD in adults is approximately 4.1%. This neurodevelopmental disorder typically begins in early childhood, with a median age of onset around 7 years. The development of ADHD symptoms tends to progress most rapidly between the ages of 7 and 9, highlighting the critical period during which the disorder becomes more apparent.
Brazil: Awareness and recognition of ADHD in Brazil have been increasing in recent years. Efforts have been made to improve the identification and diagnosis of ADHD cases, leading to greater access to appropriate interventions and support services. Finding from a 2012 study indicates that the prevalence rate of ADHD has been estimated to be 5.1%. Children diagnosed with ADHD in Brazil often exhibit higher levels of symptoms associated with the disorder.
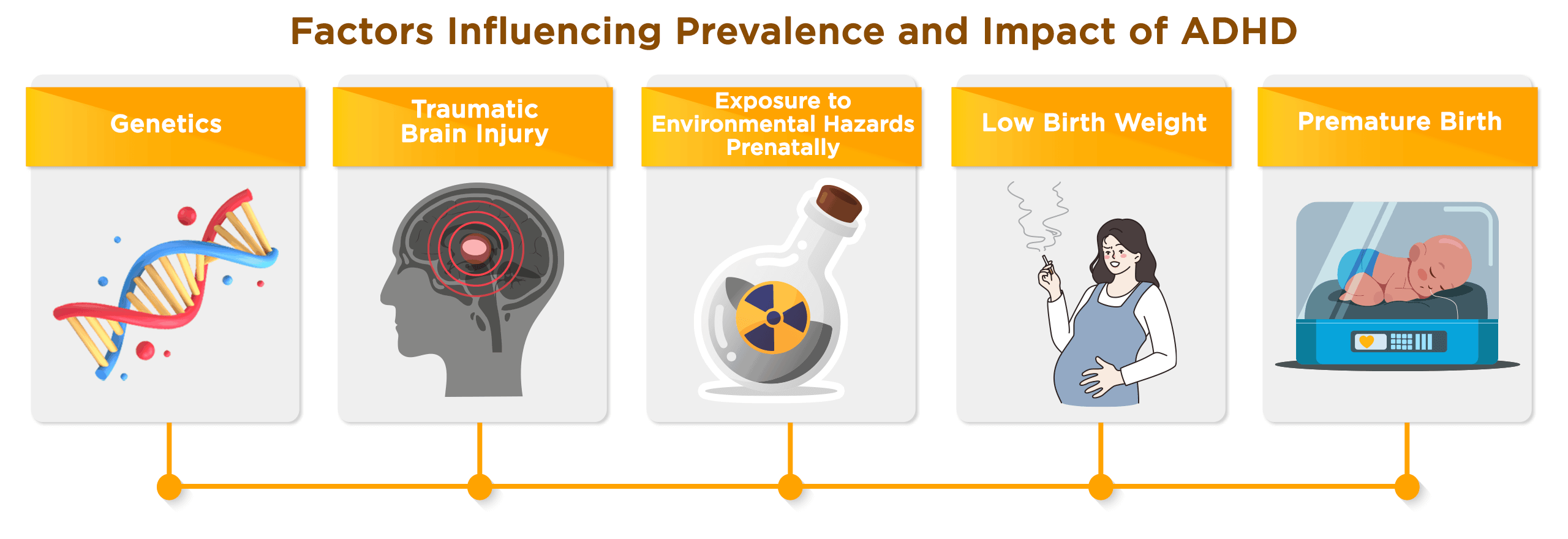
Factors Influencing Prevalence and Impact of ADHD
Manifesting as a collection of symptoms that range from hyperactivity and impulsivity to inattention, ADHD has a profound impact on an individual's cognitive and social abilities. The exact cause of ADHD remains a mystery, but it is believed to be a complex interplay of various factors.
Genetics: There is significant evidence to suggest that ADHD runs in families, indicating a strong genetic component. Recent research has shed light on the substantial genetic component of ADHD, with the heritability of the disorder estimated at roughly 80%. This percentage is notably higher than that of many other psychiatric conditions, reinforcing the significant role genetics play in the occurrence of ADHD. Moreover, research has shown that a child with a sibling diagnosed with ADHD is nine times more likely to also have the disorder compared to children whose siblings do not have ADHD.
Traumatic Brain Injury: Traumatic brain injury (TBI) is a common reason for hospital admissions among young children and adolescents. A 2021 study presented compelling evidence that the severity of traumatic brain injury (TBI) can have a substantial influence on the risk of developing ADHD. The research highlighted that children who suffered severe TBI were at an increased risk for ADHD, an association that was not as prominent in cases of mild to moderate TBI.
Exposure to Environmental Hazards (such as lead) Prenatally or in Early Childhood: Lead is a heavy metal useful in a variety of applications, including batteries, pipes, paint, and gasoline. However, it is also a potent neurotoxin that can be harmful to humans, particularly children, when ingested or inhaled. A study in Psychological Science showed for the first time that even tiny amounts of lead, like the levels often found in the U.S., can make ADHD symptoms worse in some people.
Low Birth Weight: Low birth weight is another risk factor associated with ADHD. It is hypothesized that the conditions leading to low birth weight, such as maternal smoking during pregnancy, or premature birth, might interfere with the normal development of the fetus, including the brain, thereby increasing the risk of ADHD. Numerous research findings also indicate that children who are born with a significantly low or extremely low birth weight have a likelihood up to 3.8 times greater of being diagnosed with ADHD.
Premature Birth: Prematurely born infants are at an elevated risk for ADHD. The precise reasons remain unknown, but premature birth could result in developmental delays or issues in brain development, contributing to ADHD symptoms. A particular study indicates that children born prematurely are at a heightened risk of exhibiting ADHD symptoms that may not meet the full diagnostic criteria, with the inattentive type being particularly prevalent.
Prevalence and Impact of ADHD in the United States
ADHD has a substantial influence on the lives of many individuals across the United States.
Approximately 4.4% of adults in the U.S. are affected by ADHD, with the condition being more frequently diagnosed in men, at a rate of 5.4%, compared to a 3.2% diagnosis rate in women. This rise is not just indicative of an increasing incidence but also points to a greater awareness and understanding of the disorder within the medical community and the general population.
ADHD Prevalence Across Different States
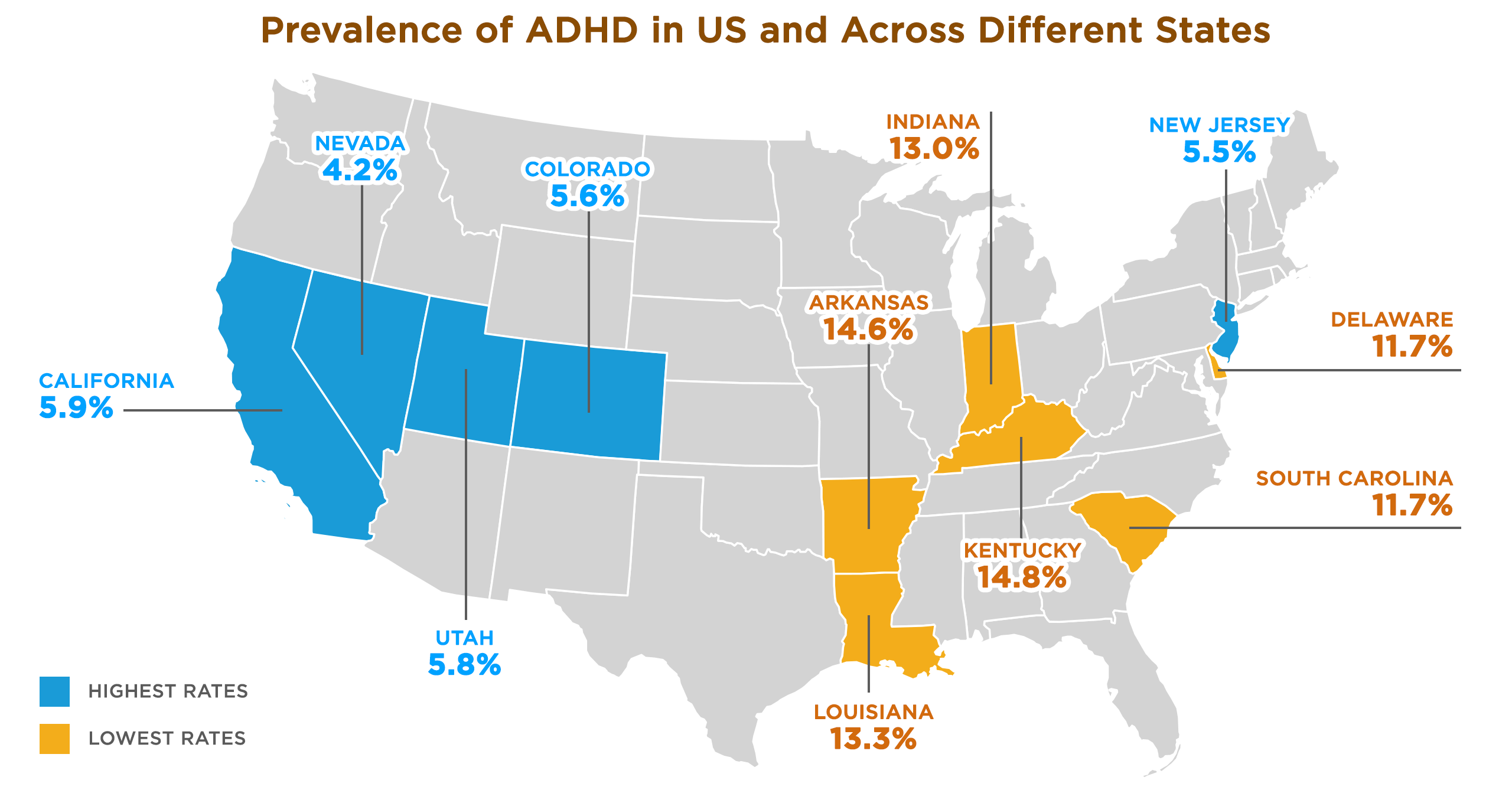
Every state in the United States, presents a unique ADHD prevalence profile, indicating that regional factors can play a significant role in shaping these patterns.
Highest Rates
A comprehensive examination of ADHD prevalence across the United States reveals a discernible pattern, with states in the Midwest seeming to have the highest rates. Notably, the state of Kentucky emerges as the one with the highest ADHD rates.
Kentucky: 14.8%
Arkansas: 14.6%
Louisiana: 13.3%
Indiana: 13.0%
Delaware and South Carolina: 11.7%
Lowest Rates
According to a study, the states in the western region of the United States, in contrast to those in the Midwest, exhibit the lowest rates of ADHD prevalence.
Nevada: 4.2%
New Jersey: 5.5%
Colorado: 5.6%
Utah: 5.8%
California: 5.9%
ADHD Prevalence by Age
No matter what age, ADHD remains a significant concern. It's a condition that can present at various stages of life, from early childhood through adolescence and into adulthood. While traditionally associated with childhood, it's now recognized that ADHD symptoms can persist into adulthood or even manifest for the first time in some adults.
Children
ADHD is often first diagnosed in childhood, making this a critical age group for understanding the disorder. It's one of the most common neurodevelopmental disorders among children. According to a national parent survey conducted from 2016 to 2019, around 6 million children aged 3-17 years, or 9.8% of this age group, have been diagnosed with ADHD at some point. Early diagnosis in this age group can facilitate timely intervention, thus improving the child's academic performance, behavior, and social relationships.
Stepping in early can help kids do better. If parents start helping with their child's problems sooner rather than later, it's more likely that they can stop the child from doing badly in school or having trouble with friends. This also keeps the child from feeling bad about themselves or getting into trouble with things like drugs or alcohol.
Adolescents
As a child with ADHD matures and transitions into adolescence and adulthood, their symptoms can shift. Based on data from the CDC, about 62% of those aged 12-17 are on medication for ADHD, and 42% have undergone behavioral therapy. Teenagers with ADHD are often more prone to act on impulse, taking part in risky behaviors such as using drugs or engaging in unsafe sexual activity.
They often have difficulty remembering assignments, misplacing textbooks, and can quickly lose interest in daily school tasks. Also, some teens may show signs of either excessive inattention or hyper-focus, impulsively answering before their turn. They might disrupt their teachers and classmates or hastily complete their assignments, and may struggle to remain seated due to restlessness.
Adults
Adults diagnosed with ADHD typically show signs of the disorder before they turn 12. In their adult life, they consistently exhibit at least five symptoms of either inattention or hyperactivity-impulsivity. Sometimes, a person may not receive an ADHD diagnosis until adulthood. This could be because their teachers or family didn't notice the symptoms when they were young, their ADHD was mild, or they coped reasonably well until the responsibilities of adulthood, especially work, challenged them.
A comprehensive review and meta-analysis of 14 different research studies, collectively comprising more than 9,400 adult participants from psychiatric outpatient clinics, reveals a significant prevalence of adult ADHD. The combined prevalence rate from the five studies that employed a two-stage design was approximately 15%. Meanwhile, the nine screening studies indicated a somewhat higher prevalence, about 27%. This research was made public in the Journal of Attention Disorders. Another research from 2019 suggested an ADHD prevalence of 0.96% in adults, which was a two-fold increase from 0.43% ten years earlier.
ADHD Prevalence by Gender
Attention deficit hyperactivity disorder (ADHD) is a condition that affects individuals across all gender identities, but the impact and expression of ADHD can vary based on each gender. ADHD tends to be more frequently diagnosed in males, but females often remain underdiagnosed or inaccurately diagnosed due to differences in how symptoms manifest. Additionally, it's important to note that ADHD also impacts the LGBTQ+ community, further highlighting the wide-reaching spectrum of individuals affected by this condition.
Male
In men, ADHD may exhibit emotional instability, sensitivity to criticism or conflict, and a tendency to evade emotionally charged situations. They are prone to react swiftly and intensely, often giving the impression of struggling with anger management. Men are nearly thrice as likely to receive an ADHD diagnosis as women, according to reliable sources. Throughout their lifespan, about 13% of men will be identified with ADHD, while the diagnosis rate for women stands at a significantly lower 4.%.
Men with ADHD often avoid conflict, get irritated easily, and find calming down challenging, which can strain relationships. They may appear messy or neglect details, leaving their partners feeling as though they're always tidying up after them.
Female
Women with ADHD are less likely to display overt hyperactivity and impulsiveness. Instead, internal hyperactivity in women may manifest as excessive rumination, intrusive thoughts, and self-deprecating talk. These symptoms can take the form of unproductive daydreaming, anxiety, depression, and a tendency to 'zone out' during conversations.
As per the data from the Centers for Disease Control and Prevention (CDC), ADHD affects 5.6% of women. The symptoms of ADHD in girls are frequently misconstrued as personal characteristics rather than indicators of a disorder. As a woman seeks assistance for these symptoms, she is often misdiagnosed with depression or anxiety rather than ADHD.
LGBTQ
Even members of the LGBTQ+ community can experience ADHD, which can bring about unique challenges in their lives. The intersection of dealing with a neurodevelopmental disorder and navigating societal attitudes towards one's sexual orientation or gender identity can amplify the difficulties they face.
Among adults who identify as lesbian, gay, or bisexual, 30% of men and 36% of women also classify themselves as having a disability. Those who identify as LGBTQ+ and those with invisible disabilities, like learning disabilities such as dyslexia, mental health issues or ADHD, face a shared decision about whether or not to disclose their status or "come out of the closet."
ADHD Prevalence by Racial/Ethnic Group
Studies report the prevalence of ADHD across racial and ethnic groups, with Black children having lower rates than non-Hispanic White children. The reasons for these disparities remain unclear but could include socioeconomic and cultural influences, differing perceptions of children's behavior, and variations in applying diagnostic criteria.
White
ADHD does not discriminate based on race or ethnicity, as it is a condition that can occur in individuals from diverse backgrounds. A study utilizing data from the National Health and Nutrition Examination Survey indicated a higher prevalence of ADHD in White children aged 12 to 15 years, with a rate of 12.65%. In addition, a significant discovery from a recent scholarly study indicates that White children are particularly prone to being overdiagnosed and excessively treated for attention-deficit/hyperactivity disorder during their elementary school years.
Black
The Black community is often disproportionately affected by various forms of discrimination, including in the context of ADHD. According to a recent meta-analysis published in JAMA Psychiatry in September, it was discovered that Black individuals have a higher likelihood of being diagnosed with ADHD compared to the general population. Additionally, a CDC study reported in March of 2020 revealed that 14% of children aged 3-17 have received a diagnosis of ADHD or a learning disability, with the percentage rising to 17% among Black children.
Asian/Pacific Islander
Over the past decade, our understanding of ADHD has significantly progressed, transforming it from a label associated with unruly behavior, particularly in schoolboys, to a recognized neurodevelopmental disorder with well-defined biological foundations. However, amidst this substantial shift, individuals from communities of color have frequently been overlooked. Recent research conducted in 2021 revealed significant disparities in ADHD diagnosis among different racial and ethnic groups. For every 100 white children diagnosed with ADHD, the study found that 83 Black children, 77 Hispanic children, and only 48 Asian children received the same diagnosis.
Hispanic
A study published in the journal Pediatrics in September 2016 revealed that Latino children exhibited ADHD symptoms at a similar rate to white children, but they were less likely to receive a diagnosis or treatment for the condition. The study found that among 10th grade children displaying the highest levels of ADHD symptoms, only 36 percent of African American children and 30 percent of Latino children with ADHD were taking medication, in contrast to 65 percent of white children. These findings highlight disparities in ADHD diagnosis and treatment, with Latino and African American children being underrepresented in receiving appropriate care compared to their white counterparts.
Native American
In comparison to Non-Hispanic White children, Non-Hispanic Alaskan Native/American Indian children have been found to have higher rates of ADHD, with a prevalence of 11.9%. A study examining the symptoms of American Indian/Alaska Native (AI/AN) boys and girls highlighted the need for affordable, evidence-based, and reliable mental health care within AI/AN families. Understanding how mental health and behavior problems manifest in AI/AN groups is the crucial first step in providing appropriate care. While it is important to acknowledge that generalizing beyond the specific sample and tribe of the study is premature, the findings suggest that AI/AN boys may exhibit higher rates of ADHD symptoms compared to AI/AN girls.
Age of Onset and Diagnosis
Although the modern understanding of attention deficit/hyperactivity disorder (ADHD) is a relatively recent development, descriptions of the typical pattern of ADHD symptoms have been documented in literature since the nineteenth century. These early descriptions consistently emphasized an early onset of symptoms. It is commonly observed that ADHD symptoms and impairments manifest during the preschool period. In many cases, ADHD symptoms begin before the age of 12, and in some children, they can even be noticeable as early as 3 years old. The severity of ADHD symptoms can range from mild to moderate or severe, and in some individuals, these symptoms may persist into adulthood.
Early Childhood Symptoms and Signs
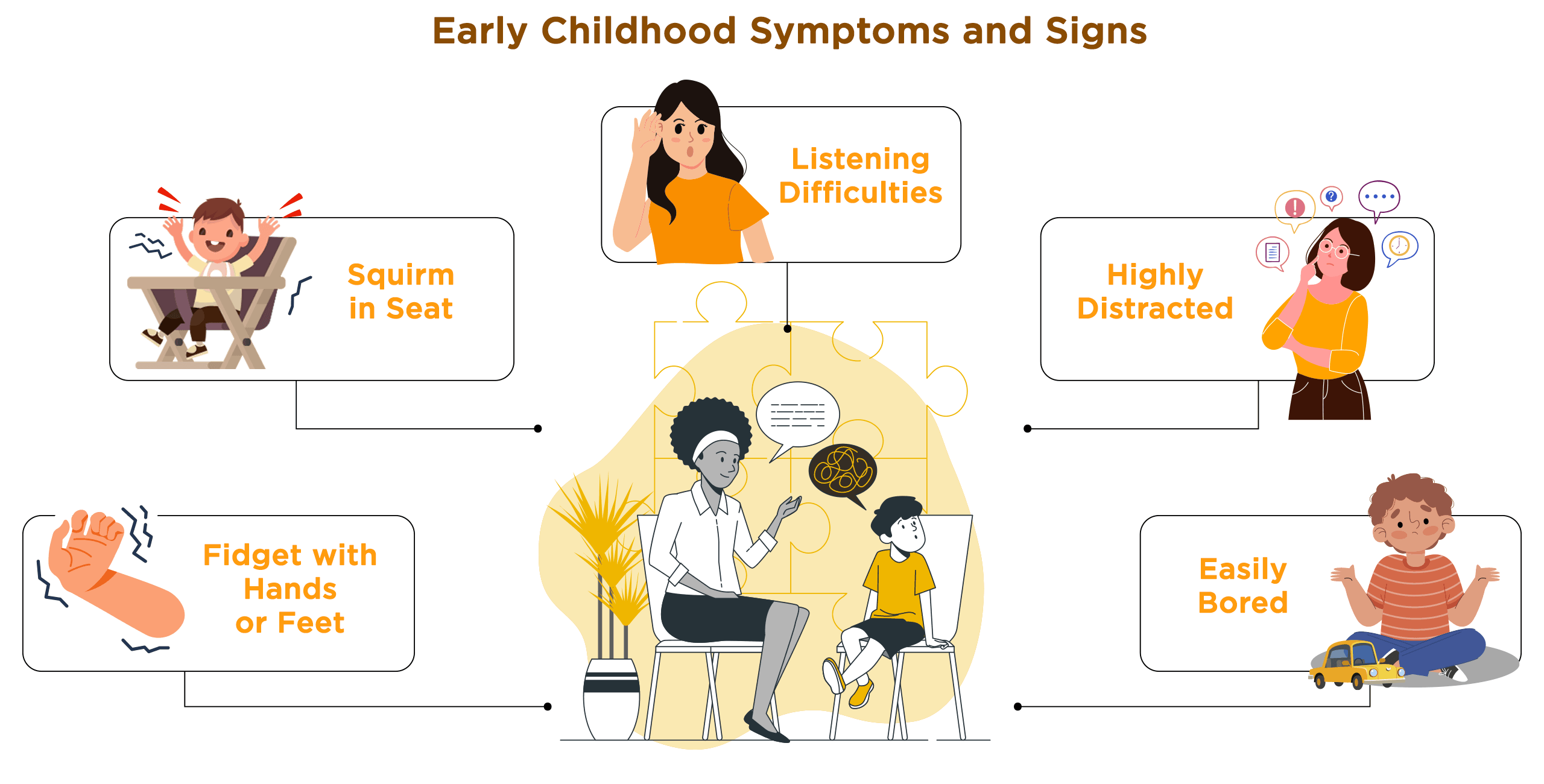
Being aware of the early childhood symptoms and signs of ADHD, parents, caregivers, and educators can better identify and address the needs of children who may be experiencing difficulties related to attention, hyperactivity, and impulsivity. Understanding these early indicators can pave the way for appropriate interventions and support to promote optimal development and well-being.
Fidget with Hands or Feet: One of the early signs of ADHD in young children is excessive fidgeting or restlessness. Contrary to common assumptions, fidgeting in individuals with ADHD actually signifies their attempt to maintain focus. It indicates that they are seeking additional stimulation because the current task at hand does not engage their brain sufficiently. Several studies have demonstrated that children with ADHD are more prone to fidgeting or seeking alternative sources of stimulation, such as playing or conversing with others, particularly in low-stimulus environments. For instance, research has shown that children with ADHD displayed better ability to sit still in a waiting room when provided with a video to watch, compared to situations where no stimulation was available.
Squirm in Seat: Children with ADHD may find it challenging to remain seated for extended periods. They may frequently squirm, shift positions, or appear unsettled in their chairs. New research indicates that squirming or movement may aid certain children with ADHD in their learning process. The study involved observing the level of movement exhibited by children while they engaged in cognitive tasks. The findings revealed that approximately 50% of the children with ADHD demonstrated notable improvements in memory-related tasks when they were permitted to move around in their seats. Additionally, a majority of the remaining children with ADHD also showed some degree of enhanced performance when given the opportunity to move.
Listening Difficulties: Children with ADHD may struggle with active listening skills. They may appear inattentive or have difficulty following instructions, particularly those involving multiple steps. They may often seem distracted, miss important details, or have trouble retaining information presented orally. Findings from a research study conducted in 2014 suggest a connection between reading comprehension difficulties in children with attention difficulties and their poor word reading skills. Additionally, the study highlighted that children at risk of ADHD are particularly susceptible to challenges in listening comprehension. These listening difficulties can impact their academic performance and social interactions.
Highly Distracted: Another early symptom of ADHD is being easily distracted. Research conducted in 2022 discovered that children with attention deficits may struggle to return to tasks after being interrupted, even if the distractor itself does not hold their attention for an extended period. While these children may not necessarily fixate on distractions for long durations, the presence of a distractor hampers their ability to maintain focus on task-relevant stimuli and reduces task performance rates. This indicates that even minor distractions can have a significant impact on their concentration, leading to challenges in completing activities and reduced productivity.
Easily Bored: Boredom, commonly experienced across neurological and psychiatric populations, remains poorly understood in terms of its cognitive characteristics. A 2012 study explored the relationship between boredom proneness, sustained attention, and adult ADHD symptoms. The findings revealed that individuals with high boredom proneness performed poorly in sustained attention tasks, exhibited increased ADHD symptoms, and could be categorized as apathetic or agitated. Apathetic boredom proneness was associated with attention lapses, while agitated boredom proneness showed reduced sensitivity to sustained attention errors and increased ADHD symptoms. The study highlights the complex relationship between attention and boredom proneness.
Diagnostic Criteria for ADHD
The process of determining whether a child has ADHD involves multiple stages and this section provides a general overview of how ADHD is identified. ADHD cannot be diagnosed with a singular test, and several other conditions, including sleep disturbances, anxiety, depression, and certain learning disorders, can present symptoms that closely resemble those of ADHD.
DSM-5 Criteria for ADHD
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) outlines the following criteria for diagnosing ADHD:
Inattention: At least six symptoms of inattention must be present for children up to 16 years old, or a minimum of five for individuals aged 17 and older; these symptoms should have persisted for at least six months and be incongruent with the person's developmental level:
Frequently overlooks details or commits careless errors in tasks at school, work, or other activities.
Regularly struggles to maintain focus on tasks or recreational activities.
Often appears unresponsive when addressed directly.
Regularly fails to carry out instructions to completion, resulting in incomplete schoolwork, chores, or duties at the workplace (for example, becomes sidetracked or loses focus).
Regularly finds it challenging to organize tasks and activities.
Frequently evades, dislikes, or is hesitant to undertake tasks requiring sustained mental effort (such as homework or schoolwork).
Regularly misplaces items required for tasks or activities (e.g., school supplies, pencils, books, tools, wallets, keys, paperwork, eyeglasses, cell phones).
Is often easily sidetracked.
Often forgets to carry out everyday tasks.
Hyperactivity and Impulsivity: For children up to 16 years old, at least six symptoms of hyperactivity-impulsivity are required, or at least five for adolescents aged 17 and older and adults. These symptoms should have persisted for at least six months and be disruptive and inappropriate relative to the individual's developmental level:
Frequently fidgets with hands or feet, or squirms in seat.
Often rises from seat in situations where sitting is expected.
Often engages in inappropriate running about or climbing (adolescents or adults may feel restless).
Frequently unable to engage in leisure activities quietly.
Often appears as if driven by a motor, constantly "on the go."
Frequently talks excessively.
Often answers before a question has been fully asked.
Frequently struggles with waiting for their turn.
Often interrupts or imposes on others (e.g., interrupts conversations or games).
Furthermore, the following conditions should be met:
Several symptoms of inattention or hyperactivity-impulsivity were present before the age of 12.
Several symptoms are present in more than one setting (e.g., home, school, work, with friends or relatives, or other activities).
Clear evidence exists that the symptoms significantly impair the quality of social, academic, or occupational functioning.
The symptoms do not solely occur during a schizophrenic or other psychotic episode. The symptoms are not better accounted for by another mental disorder (e.g., Mood Disorder, Anxiety Disorder, Dissociative Disorder, or a Personality Disorder).
Depending on the symptomatology, three presentations of ADHD can occur:
Combined Presentation: If sufficient symptoms of both inattention and hyperactivity-impulsivity criteria have been present for the past six months.
Predominantly Inattentive Presentation: If enough symptoms of inattention, but not hyperactivity-impulsivity, were present for the past six months.
Predominantly Hyperactive-Impulsive Presentation: If enough symptoms of hyperactivity-impulsivity, but not inattention, were present for the past six months.
As symptoms can shift over time, the presentation may also evolve.
Importance of a Comprehensive Evaluation for Accurate Diagnosis
The accurate diagnosis of ADHD is dependent on a comprehensive evaluation, primarily because ADHD shares symptoms with a multitude of other medical conditions and psychological disorders. This thorough evaluation not only safeguards against misdiagnosis but also aids in creating a precise and tailored treatment plan.
Differentiating ADHD from Other Conditions: In a study conducted by Dr. Adesman in 2001, it was suggested that medical professionals should take into account various potential differential diagnoses and co-existing conditions during the initial assessment of a patient exhibiting symptoms of ADHD. Despite recent debates, stimulant medications (such as methylphenidate and amphetamine preparations) continue to be the primary line of treatment for ADHD. Concerns persist regarding the overdiagnosis of ADHD and the inappropriate use of stimulants. However, not treating ADHD may lead to low self-esteem, social and academic difficulties, as well as an elevated risk of future antisocial behavior and substance abuse. Ensuring accurate diagnosis and the most effective management of this disorder may be pivotal in enhancing long-term outcomes for young individuals with this condition.
Avoiding Misdiagnosis: The risk of misdiagnosis arises due to the overlap of ADHD symptoms with those of other conditions. As per Dr. Ford-Jones, there's a valid concern about children being incorrectly diagnosed with ADHD based on factors such as relative age and gender. The ramifications of such misdiagnosis can significantly impact the child's education, health outcomes, and future well-being. Both medication and behavior management strategies have been shown to alleviate symptoms and enhance outcomes. By implementing recommendations and knowledge translation strategies for parents, educators, and healthcare professionals, a careful examination of children assessed for ADHD can reduce the rate of inappropriate diagnoses. This will ensure that factors such as relative maturity are adequately considered during diagnosis.
Proper Treatment Plan and Interventions: An effective treatment approach plays a crucial role in managing core ADHD symptoms such as inattention, hyperactivity, and impulsivity, thereby enhancing the individual's quality of life. A study released in 2015 underscores that one of the significant repercussions of undiagnosed ADHD is the absence of treatment. Leaving ADHD untreated can impose substantial psychological, financial, academic, and social strains not only on the affected individual but also on society at large, highlighting the importance of identifying and managing this disorder. Even though treatment has not demonstrated an ability to entirely rectify the developmental trajectory of those with ADHD, individuals who don't receive treatment tend to have worse long-term outcomes than those who do.
Comorbidity in ADHD
Comorbidity in ADHD refers to the simultaneous presence of ADHD along with one or more other psychiatric disorders in an individual. This is a common occurrence and significantly impacts the overall clinical picture, treatment approach, and prognosis.
Common Disorders that Occur with ADHD

Mood Disorders
These include conditions like bipolar disorder and dysthymia. Mood disorders can exacerbate the emotional difficulties often associated with ADHD, making diagnosis and treatment more complex. Numerous population and clinical studies have underscored the frequent coexistence of ADHD and Bipolar Disorder (BD). This confluence is particularly prevalent among adults, presenting a group of patients with a complex and severe clinical profile. These individuals often endure a diminished quality of life, experience an increased frequency of mood episodes, and have a higher incidence of substance abuse and dependence. Additionally, they generally face greater challenges with overall functioning.
Tics and Tourette Syndrome
Tourette syndrome is a neurodevelopmental condition marked by the presence of multiple enduring motor and vocal tics that manifest before reaching adulthood. Tics are characterized as abrupt, swift, repetitive, non-rhythmic, standardized, and involuntary motor actions or vocal utterances. TS and ADHD often co-exist together. A majority, over half of children diagnosed with TS also exhibit ADHD. Moreover, ADHD-related symptoms are observed in a significant range, from 35% to as high as 90%, of children diagnosed with Tourette Syndrome. In the context of simple tics, medical professionals often address ADHD initially as this strategy tends to bring about more substantial benefits for the child and the treatments generally have a higher efficacy. Tics might only necessitate treatment if they lead to notable complications.
Disruptive Behavior Disorder
Disruptive behavior disorders, along with untreated ADHD, have been identified as factors leading to a heightened risk of developing substance use disorders. Furthermore, adolescents who exhibit disruptive behavior disorders and ADHD are more prone to displaying aggression and hostility in their social interactions, and they face a higher probability of getting arrested. It's also proposed that the increased impulsivity typically associated with ADHD may lead to more antisocial behavior and its ensuing repercussions.
Sleep Disorder
Numerous studies have consistently found that sleep issues are prevalent among individuals with ADHD. Failing to receive sufficient sleep or needing to sleep at unconventional times that conflict with school or work schedules can lead to significant long-term implications. These may include physical health conditions, behavioral challenges, and mood fluctuations. Researchers believe one possible explanation is that ADHD can disrupt the typical sleep-wake cycle or circadian rhythm. An altered circadian rhythm may cause difficulty in falling asleep at a conventional bedtime, or result in interrupted sleep with frequent awakenings throughout the night.
Learning Disorder
While ADHD is not classified as a learning disability, studies suggest that approximately 70% of children with ADHD also have a specific learning disability, with these two conditions intersecting to make learning significantly difficult. The learning process heavily depends on the executive functions of the brain, notably the capacity to concentrate, pay attention, engage in a task, and utilize working memory. When an individual has both ADHD and a learning disability, it means they face a wide-ranging impairment of executive functions along with the deficit of specific skills needed for tasks such as reading, writing, and math.
Anxiety
There is a strong correlation between ADHD and anxiety, with up to 50% of individuals diagnosed with ADHD also having one or more concurrent anxiety disorders. Anxiety disorder represents the most common comorbidity with ADHD, significantly due to the fact that living with ADHD often involves a considerable degree of stress and worry. Those diagnosed with both ADHD and anxiety disorders generally exhibit more severe anxiety symptoms than those without ADHD. However, even adults diagnosed with ADHD who don't meet the criteria for an anxiety disorder may still experience occasional and situational anxiety in their day-to-day lives. This is primarily because of the effects of ADHD, which may lead to issues such as poor perception of time, weak working memory, and heightened emotions, all of which can induce anxiety.
Depression
ADHD and depression are conditions that often manifest concurrently. Research involving children and adolescents has indicated that individuals with ADHD, a neurodevelopmental disorder, face a higher risk of early-onset, recurrent depression compared to those without ADHD. When both ADHD and depression exist in an individual, the symptoms for each condition tend to be more pronounced than they would be if only one disorder was present. It's crucial for anyone diagnosed with both ADHD and depression to ensure that both conditions are effectively managed. In particular, proper identification and treatment of ADHD is of significant importance, as it can greatly influence the presentation of depression symptoms.
Substance Abuse
There is significant evidence indicating that adolescents with Substance Use Disorder (SUD) are more likely to have ADHD compared to the general population. For instance, in a large, multi-site study conducted by the National Institute of Health (NIH) focusing on cannabis use disorders, it was reported that ADHD was prevalent in 38% of both adolescent girls and boys. Moreover, children diagnosed with ADHD have been identified as being at a heightened risk of developing an SUD. The risk of SUDs has been proven to be twice as high among individuals with ADHD, and quadruple among those who have both ADHD and an accompanying conduct disorder.
Consequences and Implications of ADHD
The consequences of ADHD can be far-reaching, affecting various aspects of an individual's life such as academic performance, occupational functioning, relationships, and overall quality of life. The following section explores the significant impact of ADHD, underscoring the necessity of its timely diagnosis and effective management.
Economic Impact
ADHD is associated with a substantial economic burden that stretches across multiple dimensions of society including families. This includes costs related to the medical care and treatment of ADHD, such as diagnostic services, hospitalizations, medications, and outpatient visits. In a study conducted in 2018, the overall additional annual societal costs related to ADHD were projected to be approximately $19.4 billion for children, which equates to $6,799 per child. Similarly, for adolescents, these excess costs were estimated to be around $13.8 billion, translating to $8,349 per adolescent.
Cost of ADHD Diagnosis: The cost of ADHD diagnosis can vary widely, influenced by who performs it and whether it includes neuropsychological testing. Prices can range from hundreds to thousands of dollars. Despite being available at public clinics, there can be long wait times for appointments. For instance, at the University of Washington, a comprehensive evaluation testing academic and cognitive functioning could cost around $3,700 to $4,500 without insurance, while a brief ADHD evaluation might be around $650. Such costs can be prohibitive for many individuals and families.
Economic Burden on Families: Based on a study from 2019, it was found that the total economic strain on families raising children with ADHD was over five times higher compared to those without ADHD (average cost for ADHD was $15,036 per child, compared to $2,848 per child for those without ADHD). This considerable difference in cost remained significant even after taking into account factors such as intellectual functioning, symptoms of oppositional defiance, or conduct problems. Parents of children with ADHD were found to have more job changes, experienced job loss more frequently, and reported decreased work efficiency.
Impact on Healthcare Systems: The healthcare costs associated with ADHD can be quite substantial. They include not only the costs for diagnostic assessments, but also ongoing costs for medication, behavioral therapy, counseling, and other treatments. It's been discovered that the annual medical expenses of adults diagnosed with ADHD are significantly higher compared to their non-ADHD counterparts. Healthcare costs for adults with ADHD typically fluctuate between $4,929 and $5,651, whereas for those without the disorder, the costs are estimated to be significantly lower, ranging from $1,473 to $2,771.
Academic Performance
ADHD can hinder a student's concentration, attentiveness, and engagement in school activities, leading to disruptive behavior. Many children with ADHD, possibly having undiagnosed learning disabilities, may struggle academically before their condition is identified.
Less Confidence: People with ADHD often grapple with issues of self-worth, driven by difficulties with concentration and task completion, potentially leading to a sense of failure or deficiency. Numerous studies assessing the self-esteem of children and adolescents with ADHD have consistently found lower self-esteem in these individuals compared to their peers without ADHD. This underscores the need for early identification and support for mental well-being in these youngsters, which could help mitigate the long-term effects of ADHD symptoms.
Boredom: Experiencing boredom is an undeniable part of human existence. Despite its discomfort and our instinctive efforts to steer clear from it, boredom remains inevitable, particularly among individuals with ADHD. Studies indicate that individuals with ADHD frequently report experiencing more bouts of boredom than others. While boredom is unlikely to have fatal consequences, it can chip away at one's overall satisfaction in life and can pave the way for other problematic behaviors and situations. Research also implies that boredom can negatively impact performance at work or school.
Short Attention Span: One of the key characteristics of ADHD is a short attention span, making it difficult for individuals with the condition to focus on tasks for extended periods. A study from Austin Peay State University has shown that inadequate attention predicts diminished time spent actively engaged in academics, which subsequently results in lower grades and increases the likelihood of school failure. Regrettably, around 7.8% of U.S. children aged between 4 and 17 grapple with significant attention issues. While boys are typically affected at a ratio of 3 to 1 compared to girls, it's believed that the number of girls with attention problems is likely underreported.
Career and Employment
The workplace is a significant arena for many individuals, serving as a source of income, a platform for career advancement, and a hub for social interaction. For most, navigating this space comes with its share of complexities and demands. However, for individuals with ADHD, the workplace may pose additional hurdles, rendering it a challenging environment to manage effectively.
Tardiness: One of the prominent characteristics of ADHD is difficulty with time management. This can often result in consistent tardiness, as individuals may struggle with estimating how long tasks will take, planning their day effectively, or simply getting distracted and losing track of time. In a professional environment, chronic lateness can negatively impact one's reputation and relationships with colleagues and supervisors. Additionally, being frequently late can lead to missed meetings or deadlines, which may affect overall job performance and opportunities for advancement.
Interpersonal Conflict: ADHD can affect more than just an individual's ability to focus or stay organized. It can also lead to impulsivity, emotional dysregulation, and trouble with self-control, all of which can make interpersonal relationships challenging. In the workplace, this might manifest as difficulty in managing conflicts, tendency to interrupt or speak out of turn, or reacting emotionally in stressful situations. These behaviors can create tension between coworkers and supervisors, leading to a less harmonious and productive work environment.
High Error Rate: Concentration difficulties that come with ADHD can make it hard for an individual to pay attention to details, follow complex instructions, or stay focused on a task for extended periods. As a result, individuals with ADHD may make more mistakes in their work than their peers. This high error rate can impact the quality of work they produce and lead to reduced efficiency or productivity. In certain jobs, such as those involving safety-critical tasks, a high error rate can have severe consequences.
High Absenteeism: ADHD might also contribute to increased rates of absenteeism. This could be due to a variety of reasons: associated conditions like anxiety or depression that make it harder to maintain a regular work schedule, the need to attend frequent medical or therapy appointments, or the challenges inherent in ADHD like impulsivity and disorganization that make it harder to maintain consistent attendance. Chronic absenteeism can lead to decreased productivity, strained relationships in the workplace, and potential job loss. It also poses a burden on the individual with ADHD, as they may face financial instability and loss of job security.
ADHD and COVID-19
The COVID-19 pandemic has been tough for everyone, but it's been extra hard for people with mental health conditions like ADHD. They have found it particularly tough to adjust to the many changes brought by the pandemic. In the 2020 ADDitude's 13 surveys conducted during the pandemic, the large number of fresh ADHD diagnoses was measured. Out of 2,365 adults who took part in the survey, 26.5% stated they were formally diagnosed with ADHD in the past year.
Impact of the Pandemic on ADHD Diagnosis and Treatment
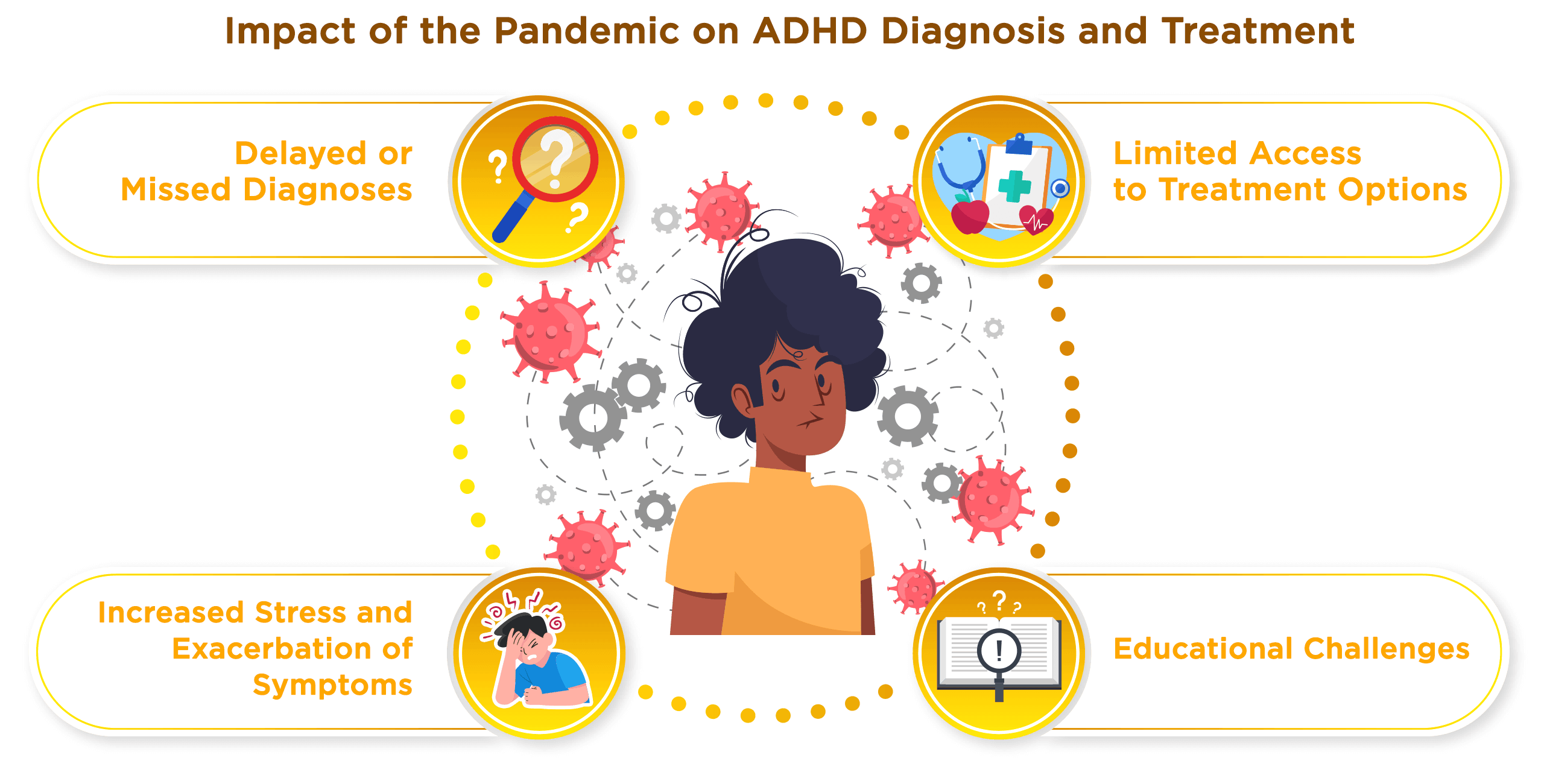
The COVID-19 pandemic has heightened the struggles faced by individuals with ADHD due to the sudden shift to online learning, disrupted routines, and increased anxiety. Closures of clinics and the transition to telehealth services may cause delays in diagnosis and limit access to necessary treatments.
Delayed or Missed Diagnoses: The pandemic's unprecedented strain on healthcare resources led to a significant diversion of focus away from routine screenings and diagnoses. Many children and adults who might otherwise have been assessed for ADHD did not receive timely evaluations. People with ADHD possess certain risk factors that could potentially heighten their susceptibility to the adverse health impacts of the pandemic. This could in turn affect the effectiveness of their treatment and their ability to stick to it. Telemedicine, however, is seen as a potentially effective tool in monitoring ADHD treatment during such challenging times.
Limited Access to Treatment Options: The sudden and necessary shift towards telemedicine presented challenges for individuals with ADHD. While telehealth offers certain advantages, like convenience and the comfort of one's home, it does not fully replace in-person consultation, particularly for behavioral therapies. Furthermore, the pandemic significantly impacted the postponement of new patient assessments as well as delays in initiation and optimization of medication.
Increased Stress and Exacerbation of Symptoms: The pandemic brought about abrupt and substantial changes in day-to-day living, creating an environment of heightened stress and uncertainty. These stressors can intensify ADHD symptoms, making them harder to manage. Increased impulsivity, difficulty focusing, restlessness, and mood fluctuations became more prominent for many individuals, especially children. The impact was even more profound if the individual had coexisting mental health conditions like anxiety or depression.
Educational Challenges: The abrupt transition to remote learning posed significant challenges for students with ADHD. Virtual classrooms lack the structured environment and immediacy of feedback that in-person schooling provides, making it harder for these students to stay engaged and focused. Additionally, parents often found it challenging to fill the role of both caregiver and educator, particularly if they were balancing work-from-home responsibilities. Parents with ADHD children often face personal mental health challenges and increased stress related to parenting. Particularly for parents of teenagers with ADHD, providing the necessary structure, organization, communication with educators and school staff, and educational guidance during remote learning can be exceedingly challenging.
Treatment Approaches for ADHD
Various methods are available to alleviate ADHD symptoms, encompassing everything from prescribed medication and therapeutic interventions to adjustments in daily routines such as prioritizing ample sleep.
How ADHD Medications Work
ADHD medications work primarily by influencing the brain's chemistry. Medications are often the primary treatment approach for ADHD, proving to be successful in managing the condition in approximately 80% of affected children.
Antidepressants: Antidepressants are medications prescribed primarily for managing depression. However, they are also utilized in treating a variety of other health conditions like treating adults with ADHD. They work by affecting neurotransmitters, which are chemicals in the brain that carry signals between nerve cells. Certain antidepressants, including imipramine, desipramine, and bupropion, have shown efficacy in managing not only major depressive disorders and anxiety conditions, but also ADHD in adult patients.
Stimulants: Stimulant medications like amphetamines (for instance, Adderall) and methylphenidate (like Ritalin and Concerta) are frequently recommended for the treatment of individuals diagnosed with ADHD, regardless of their age group - children, teenagers, or adults. The combination of these stimulants and psychotherapy often proves beneficial in alleviating the symptoms of ADHD, while also enhancing the patient's self-confidence, cognitive abilities, and interactions within their social circles and families.
Non-stimulants: Nonstimulant ADHD medications include norepinephrine modulators and alpha agonists. The most commonly prescribed nonstimulant medication is Atomoxetine (Strattera), a norepinephrine modulator, along with a recent addition called Viloxazine (Qelbree). Alpha agonists such as Clonidine (Catapres, Kapvay) and Guanfacine (Tenex, Intuniv) are also frequently used. Substantial research and data back the effectiveness of non-stimulants in treating ADHD. While stimulants are still the first-line treatment, the usage of non-stimulants is on the rise, particularly in cases where stimulants do not sufficiently address the symptoms, aren't well-tolerated by the patient, or when there are specific reasons preventing the use of stimulants.
Therapy
Therapy is a crucial part of the multi-faceted approach to managing ADHD. By utilizing various therapeutic techniques, individuals with ADHD can learn to manage their symptoms, cope with challenges, and improve their daily functioning.
Behavioral Therapy for Children: If your child is diagnosed with ADHD, it's likely your healthcare professional will suggest behavior therapy as an initial form of treatment, regardless of your child's age. This approach is widely acknowledged as the first line of defense in effectively dealing with ADHD symptoms. In 2022, a study examined the effectiveness of Cognitive Behavioral Therapy (CBT) and Methylphenidate (MPH) in managing ADHD symptoms in children and adolescents and improving their functional capabilities. After reviewing data from 2,098 patients who received one or both treatments, the researchers found a substantial decrease in core ADHD symptoms. This led to better behavior, improved functioning, and consequently, a lesser societal and familial burden.
Cognitive Behavioral Therapy for Adults: CBT is a form of therapy that aids in dealing with challenges encountered in school, work, and interpersonal relationships. CBT, with or without medication, can enhance well-being and simplify daily living. The therapy is based on the understanding that many issues arise from inaccurate or negative thoughts, and it helps you recognize how these negative thoughts create hurdles in your life. By learning to replace these false beliefs with accurate ones, improvement can be achieved. Recent studies have shown that CBT, when combined with medication, can lead to greater improvements in ADHD symptoms, organizational abilities, and self-esteem than CBT alone.
Play Therapy: Play therapy, which harnesses the power of play as a means of communication, can be a powerful tool for children with ADHD. It offers a safe and therapeutic space where children can freely express their emotions through toys, instead of struggling with words. This method has proven its worth; a 2012 study demonstrated notable reductions in ADHD symptoms among children who participated in play therapy, suggesting that it could serve as a highly effective approach to managing this condition.
Art Therapy: Art therapy, which encourages non-verbal expression and communication, can significantly benefit individuals with ADHD. Engaging in art stimulates the brain, increasing dopamine levels, which are crucial for enhancing concentration. Furthermore, the creative process can boost serotonin and reduce stress levels. According to 2003 research, art therapy can help manage ADHD symptoms by providing opportunities for social interaction, skill practice, and learning enhancement through visual and graphomotor experiences. This approach could, therefore, serve as a valuable tool for tackling attention and hyperactivity issues.
Equine Therapy: Equine therapy involves hands-on interaction with horses, supervised by a mental health professional and an equine expert, as a form of therapeutic experience, instead of traditional talk therapy. A pilot study conducted in 2011 suggested that such therapy positively influenced multiple areas of social behavior, quality of life, and motor performance in five children with ADHD. The direct engagement with horses offers a unique therapeutic approach that may benefit those with ADHD.
Support
Being diagnosed with ADHD is not a sentence to struggle or underachievement. Instead, it marks the beginning of a journey towards understanding and managing a condition that makes one's brain wired differently. With appropriate support, whether from healthcare professionals, family, friends, or ADHD-specific resources and communities, individuals can not only cope with ADHD but also leverage its unique aspects to their advantage.
Support Groups: Support groups provide a nurturing space for individuals to exchange personal stories, learn tactics to manage symptoms, and bond with others who are familiar with the complexities of living with attention deficit hyperactivity disorder (ADHD). ADHD support groups are collaborative networks of individuals united in their efforts to provide mutual support, exchange life experiences, and share insights about managing ADHD. Support groups can be found through various organizations including the Attention Deficit Disorder Association (ADDA), Children and Adults with Attention-Deficit/Hyperactivity Disorder (CHADD), and ADDitude magazine.
Parent Training and Education: The process of training and educating parents is a critical part of managing ADHD. This typically involves teaching parents effective strategies to handle ADHD-related behaviors, understanding their child's condition, and learning how to respond to their child's needs effectively. Multiple studies have revealed that enhancements in parenting practices can directly lead to positive changes in a child's ADHD behaviors. However, it's crucial to note that if negative parenting behaviors such as severe or inconsistent discipline persist, parent training tends not to result in improvements in a child's conduct. Therefore, reducing these negative parenting practices is essential for the effectiveness of parent training programs for children with ADHD.
Family Support and Communication: Family support is crucial in managing ADHD, fostering a supportive environment through open communication and understanding. This can enhance positive outcomes for those with ADHD. Studies indicate that a significant link between ADHD symptoms and depression, emphasizing that a lack of family support can contribute to the risk of developing depression alongside ADHD symptoms. Thus, strong family support is essential to alleviate the challenges associated with ADHD.
Breaking the ADHD Stigma
Breaking the ADHD stigma involves fostering awareness, enhancing knowledge, and encouraging empathy. Addressing common misconceptions and stereotypes surrounding ADHD can empower individuals with the condition and enlighten society. The following are what you can do to help reduce stigma and foster a more supportive and understanding environment for individuals with ADHD:
Sharing Your Story: Personal narratives have a unique power to illuminate the realities of living with ADHD. These stories can foster understanding, dispel myths, and provide solace to those sharing similar experiences. There's an article titled "Online Narratives by Adults With ADHD Who Were Diagnosed in Adulthood" that shares the real-life stories of adults living with ADHD. These stories allow us to understand what these individuals go through before and after they are diagnosed with ADHD, from their own point of view. The article found that these individuals often faced many failures in different areas of their life. Later on, many of them started to think more positively about themselves and their lives, even seeing some good sides of having ADHD.
Information About Treatment: Spreading accurate information about ADHD treatment options can help reduce the fear and misconceptions associated with medication and therapy. This can also support informed decisions for individuals with ADHD and their families. An article in Current Psychiatry Reports suggests that spreading accurate knowledge about ADHD can help reduce stigma and misunderstandings about the potential long-term effects of medication. This need for mental health education isn't just for healthcare professionals, but also for educators and other trusted individuals that parents and young people turn to for guidance and answers.
Sharing Research Findings: Stigma surrounding ADHD can discourage individuals and their caregivers from seeking help, resulting in delayed diagnoses and treatment. As suggested by a 2015 research review, untreated ADHD can lead to numerous adverse consequences. Publicizing the latest scientific discoveries about ADHD can highlight the complexity of the condition and the progress being made in understanding and treating it. This can provide hope to those affected and challenge outdated or misguided beliefs about ADHD.
Reputable Learning Resources: Richard Burch suggests that stigma and misconceptions about ADHD can be minimized by enhancing understanding about the causes of ADHD and how it affects the lives of those who have the disorder. Directing people towards reliable sources of information can facilitate greater understanding of ADHD. This can help both those diagnosed with ADHD and wider society to comprehend the challenges of the condition, paving the way for acceptance and support.
Positive Outcomes and Successful Coping Strategies
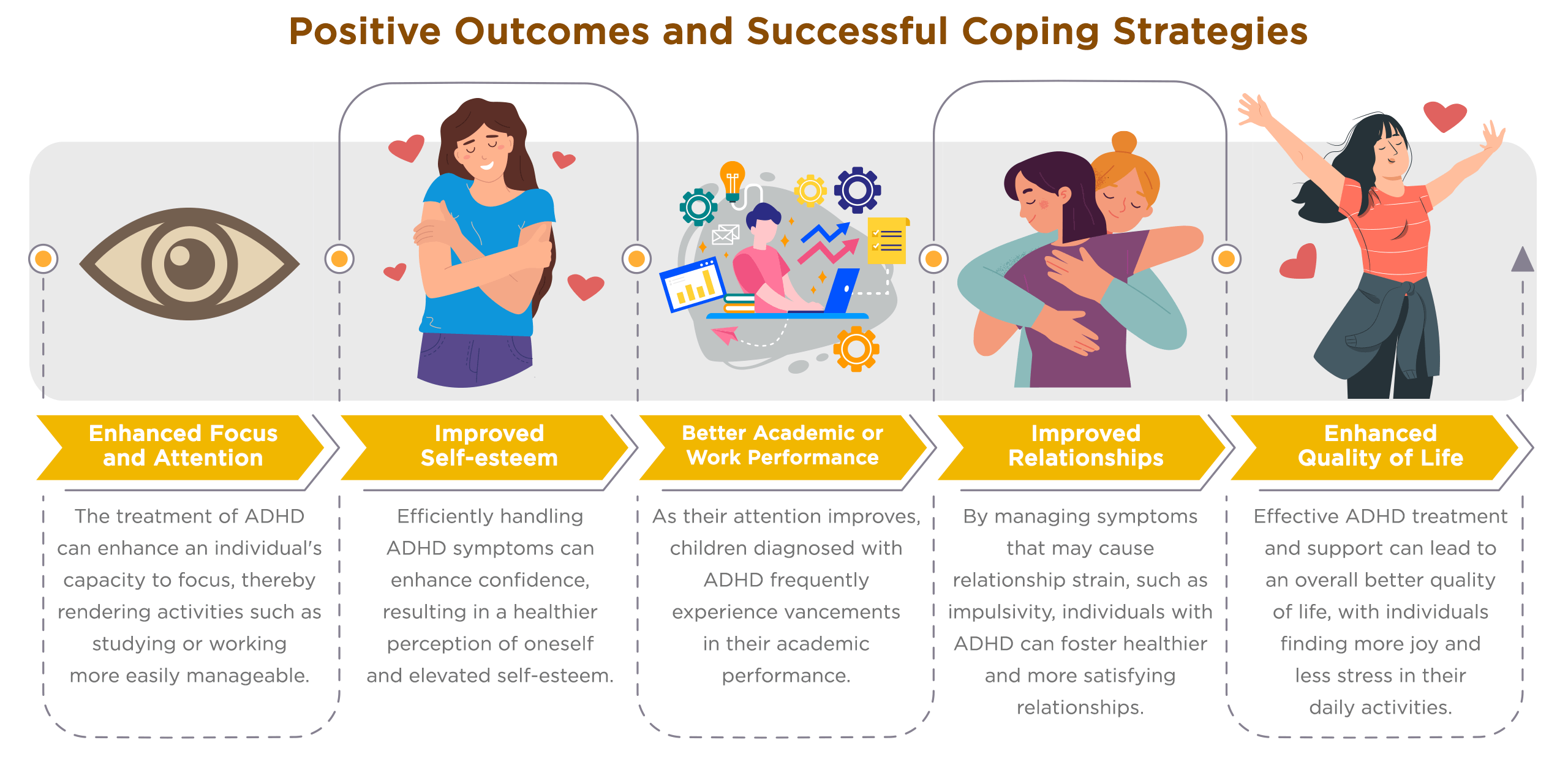
Managing ADHD effectively can open up a world of potential for those living with the condition. Embracing a range of coping strategies, alongside appropriate treatment, can lead to numerous positive outcomes, enhancing personal, academic, and professional success.
Enhanced Focus and Attention: ADHD treatment can help improve an individual's ability to concentrate, making tasks like studying or working more manageable. Medications, like stimulants, have proven to be a reliable method for managing ADHD symptoms like impulsivity, hyperactivity, and difficulty maintaining attention. These medications have shown success in about 70% of adults and between 70-80% of children with ADHD. They are particularly effective at minimizing disruptive behaviors and reducing excess energy or restlessness.
Improved Self-esteem: Managing ADHD symptoms effectively can boost confidence, leading to a healthier self-image and improved self-esteem. For example, the performing art of magic, when used as a form of therapy, has been demonstrated to boost self-confidence in children with neurodevelopmental disorders. Assisting them in refining their craft and lending support can significantly influence the development of their personalities and boost their self-confidence. This empowerment can make them more resilient and proactive in managing their condition and navigating daily life, ultimately contributing to their overall well-being.
Better Academic or Work Performance: With improved attention, children with ADHD often see improvements in their schoolwork. They may need additional support, like extra time on tests, but with the right strategies and accommodations, they can achieve their academic goals. ADHD can negatively impact long-term academic results. However, studies have shown that a higher percentage of outcomes on achievement tests see improvements with treatment as compared to overall academic performance. These improvements are most consistently seen when various treatments are combined, offering a holistic approach to managing ADHD.
Improved Relationships: By managing symptoms that may cause relationship strain, such as impulsivity, individuals with ADHD can foster healthier and more satisfying relationships. Just as encouraging academic strengths can help, aiding children and young people with ADHD to build strong family ties and friendships seems to create a supportive social environment. This approach helps in fostering protective factors in interpersonal relationships, potentially leading to a greater sense of social support.
Enhanced Quality of Life: Effective ADHD treatment and support can lead to an overall better quality of life, with individuals finding more joy and less stress in their daily activities. The early identification and medication-based management of ADHD can greatly improve outcomes, long-term outlook, and overall life quality for adults living with this condition. This improvement stems from better control over ADHD symptoms, leading to fewer disruptions in day-to-day activities and more fulfilling personal and professional relationships
The Final Thoughts: Impact and Need for ADHD Awareness and Support
The substantial impact and need for ADHD awareness and support is clear. ADHD presents a considerable challenge to those living with it, influencing every aspect of their lives, from academic and professional success to personal relationships and self-esteem. The collective investment in strengthening ADHD awareness, fostering supportive systems, and improving treatment approaches is crucial in turning these challenges into potential assets. By eliminating related stigmas, sharing personal narratives, and distributing accurate information, we can create a compassionate environment that enables individuals with ADHD to flourish.
The latest advancements in neuroimaging, genetics, and medication are promising. These tools and resources are contributing to our understanding of ADHD, leading to more accurate diagnoses and better treatment options. It is hoped that further research will continue to shed light on this complex disorder, allowing for improved quality of life for those affected by ADHD and those around them.
Recommended Articles





